Viruses are microscopic organisms that require a living host to multiply and survive, and throughout history, they have caused widespread illnesses, sometimes with very high mortality rates. Some viruses, like the influenza virus, are common, with strains that evolve and spread globally each year. Rare but highly lethal viruses, such as the Marburg virus, have also emerged. Despite advances in medical science, these pathogens remain a significant threat to human health, and understanding them is crucial for developing effective preventive measures and treatments.
The risk posed by viral pathogens varies by the virus, the mode of transmission, and the availability of treatment or vaccines. Diseases such as HIV/AIDS have had a profound impact on global health, while the emergence of coronaviruses like SARS-CoV and SARS-CoV-2 has demonstrated the rapidity with which new viruses can spread across the globe as per Medical News Today. Vaccination and other control measures have successfully reduced the spread and severity of some viral infections, but others, such as Ebola and rabies, continue to pose serious challenges to public health.
Key Takeaways
- This discussion has highlighted a range of viruses, including HIV/AIDS, Influenza, Coronaviruses (SARS-CoV, MERS-CoV, SARS-CoV-2), Hepatitis (A, E, B, C), Rabies, Hantaviruses, Dengue, Marburg, Nipah, and Crimean-Congo Hemorrhagic Fever Virus, each presenting unique challenges and implications for global health.
- The impact of viruses is multifaceted, affecting not only individual health but also economic, social, and developmental aspects of societies.
- Viruses can be highly lethal and are a constant threat to public health.
- Their impact is influenced by their transmission modes and the existence of treatments or vaccines.
- Ongoing research and preventive strategies are critical in combatting viral diseases.
Viral Pathogenicity
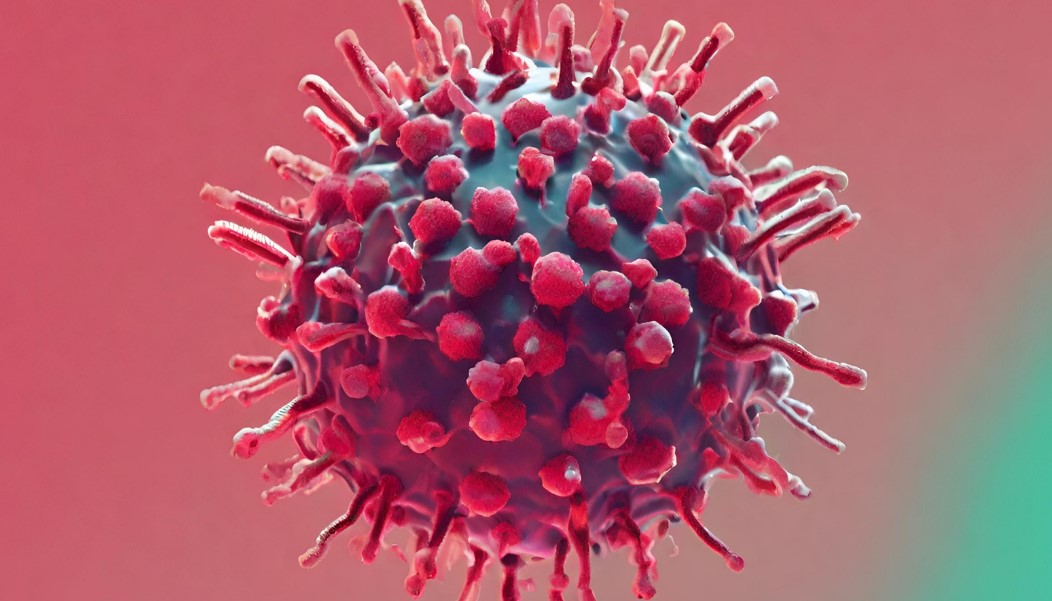 Pathogenicity refers to the ability of a virus to cause disease in a host organism according to a study from Tulane University. I understand that this disease-causing potential varies widely among different viruses, influenced by factors such as viral structure, mode of transmission, and the intrinsic properties of the virus.
Pathogenicity refers to the ability of a virus to cause disease in a host organism according to a study from Tulane University. I understand that this disease-causing potential varies widely among different viruses, influenced by factors such as viral structure, mode of transmission, and the intrinsic properties of the virus.
- Viral Structure: The complexity of a virus’s structure, including its genetic material (DNA or RNA) and protein coat (capsid), can determine how effectively it invades host cells as noted by the National Institute of Health.
- Mode of Transmission: The way a virus spreads can be a factor. Some are airborne, others transmit through bodily fluids, and some by vector organisms.
Host Factors: A host’s immune response plays a crucial role in the impact of a pathogen. Comorbidities and genetic predisposition can amplify a virus’s effect also noted by the NCBI.
Furthermore, a virus’s replication rate is also a determining factor—viruses that replicate quickly can outpace the host’s immune response.
| Factor | Influence on Pathogenicity |
|---|---|
| Viral Load | Higher loads can lead to more severe disease. |
| Cell Tropism | Specificity for certain cell types affects outcome. |
| Immune System Evasion | Ability to avoid immune detection enhances virulence. |
In summary, the pathogenicity of a virus encapsulates its capability to cause harm, which arises from an intricate interplay of viral characteristics and host vulnerabilities. Understanding these factors is vital for developing preventive and therapeutic measures.
Modes of Virus Transmission
Understanding how viruses spread is crucial in preventing and controlling outbreaks. Different viruses have specific paths of transmission which can include air, animal vectors, or direct contact.
Airborne Transmission
Airborne transmission occurs when infectious agents are carried by dust or droplet nuclei in the air. Influenza and the common cold are typical examples where viruses spread through coughing or sneezing according to Cleveland Clinic.
Vector-Borne Transmission
Vector-borne transmission refers to the spread of viruses through organisms such as mosquitoes or ticks. One well-known case is the Zika virus, which is primarily spread by Aedes mosquitoes.
Direct Contact Transmission
In this part, I will indicate that direct contact transmission includes the physical transfer of microbes through touch. The Marburg virus can be spread from person to person through contact with bodily fluids of infected individuals according to WHO.
Factors Influencing Virulence
 When assessing the danger posed by viruses, it’s imperative to understand the factors that influence their virulence. Virulence refers to the degree of damage a virus can cause to its host. As a biologist, I highlight several factors essential in determining a virus’s virility.
When assessing the danger posed by viruses, it’s imperative to understand the factors that influence their virulence. Virulence refers to the degree of damage a virus can cause to its host. As a biologist, I highlight several factors essential in determining a virus’s virility.
Genetic Makeup
The genetic variability of a virus can result in strains with differing levels of virulence. For instance, certain influenza A viruses exhibit a broad spectrum of virulence, from those causing mild symptoms to others that are potentially lethal.
Transmission Mechanisms
How a virus transmits can affect its virulence. Viruses that spread through respiratory droplets, for example, may evolve to cause less severe symptoms to optimize their spread.
Host Factors
- Age
- Immune system strength
- General health
- Presence of comorbidities
These host factors determine an individual’s susceptibility to severe viral infections and the subsequent complications.
Environmental Influences
- Climate
- Population density
- Hygiene practices
Such environmental factors can affect the rate and ease with which a virus spreads, thereby impacting its overall virulence.
I also take note of virulence factors like adhesion mechanisms, which allow viruses to attach to and invade host cells, and antigenic variation, enabling them to evade immune responses. These are well-documented in the mechanisms viruses use for adhesion and antigenic variation.
Lastly, the presence and function of viral proteins that can subvert host defenses significantly contribute to pathogenicity. Understanding these factors is crucial in developing strategies to combat viral infections and mitigate their impact on public health.
1. Ebola Virus
Ebola virus is among the most lethal pathogens, known for causing severe hemorrhagic fever in humans and a high fatality rate. Outbreaks of Ebola have caused significant loss of life and sparked worldwide concern according to a study from NCBI.
History of Ebola Outbreaks
The first recorded outbreak of Ebola virus disease occurred in 1976 in two simultaneous incidents, one in Sudan and the other in the Democratic Republic of Congo (DRC), which was then known as Zaire as noted by the CDC. Since then, the DRC has experienced multiple outbreaks, the most notable one beginning in 2014, which became the largest Ebola outbreak in history, spreading across borders and raising global alarms.
Ebola Virus Disease Symptoms
Symptoms of Ebola virus disease (EVD) typically begin abruptly within 2 to 21 days after infection. Early symptoms resemble the flu and include:
- Fever
- Severe headache
- Muscle pain
- Weakness
- Fatigue
As the disease progresses, it can cause:
- Vomiting
- Diarrhea
- Rash
- Impaired kidney and liver function
In some cases, patients may experience:
- Internal and external bleeding (e.g., bleeding from the gums, blood in the stools)
Prevention and Treatment
There is no FDA-approved cure, but early, supportive care with rehydration and symptomatic treatment improves survival. Researchers have developed an Ebola virus vaccine that provides a high degree of protection and which was used effectively in the 2018 DRC outbreak also stated by the CDC. Prevention methods include:
- Avoiding contact with the blood and bodily fluids of people displaying symptoms
- Wearing protective clothing and equipment when handling patients
- Implementing quarantine measures effectively
In 2018, the DRC faced a significant Ebola outbreak in its eastern region. This outbreak posed unique challenges due to the region’s complex security situation and the dense, mobile population. However, it also marked a significant advance in the fight against Ebola.
For the first time, a newly developed vaccine, rVSV-ZEBOV, was deployed on a large scale. Over 300,000 people were vaccinated, including frontline healthcare workers and contacts of confirmed cases. This vaccination campaign, combined with traditional containment strategies like contact tracing, quarantine, and public health education, proved instrumental in controlling the outbreak.
2. HIV/AIDS
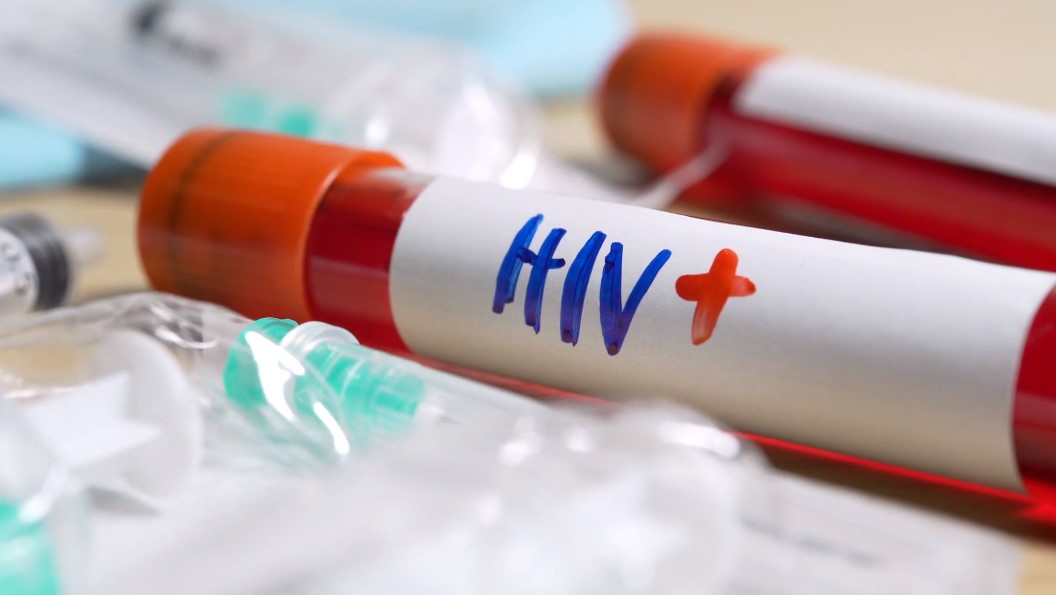 I’ve come to understand the significant burden HIV/AIDS has on global health. The Human Immunodeficiency Virus (HIV) leads to Acquired Immunodeficiency Syndrome (AIDS), a condition that compromises the immune system, allowing for opportunistic infections and cancers to thrive according to HIV.gov.
I’ve come to understand the significant burden HIV/AIDS has on global health. The Human Immunodeficiency Virus (HIV) leads to Acquired Immunodeficiency Syndrome (AIDS), a condition that compromises the immune system, allowing for opportunistic infections and cancers to thrive according to HIV.gov.
Global Impact of HIV/AIDS
I’ve analyzed data which shows that HIV continues to be a major global public health issue. It’s estimated that about 37.7 million people were living with HIV in 2020, and despite the global efforts, approximately 1.5 million new cases are still reported annually.
The virus has had a profound impact, especially in Sub-Saharan Africa, where a large percentage of cases are concentrated. HIV not only affects the health of individuals, but it also imposes a significant economic burden on affected countries referring to a study from BMC Public Health.
Advancements in HIV Treatment
The medical community has made substantial progress in treating HIV. Antiretroviral therapy (ART) has transformed HIV from a fatal diagnosis to a manageable chronic condition for many. Patients receiving effective ART can achieve an undetectable viral load, significantly reducing the likelihood of transmitting the virus to others noted by the Oxford Academics. The introduction of pre-exposure prophylaxis (PrEP) is another landmark in prevention, offering high-risk individuals a means to significantly decrease their risk of contracting HIV.
Challenges in HIV Prevention
Despite major treatment advances, there are considerable challenges remaining in HIV prevention. Stigma continues to hinder testing and treatment, particularly in certain regions of the world. Furthermore, the need for daily medication presents adherence challenges, and there’s a critical need for increased access to healthcare services to ensure those living with HIV receive continuous care. Diverse strategies, tailored to meet the needs of varying populations, are essential for effective prevention efforts moving forward.
3. Influenza Virus
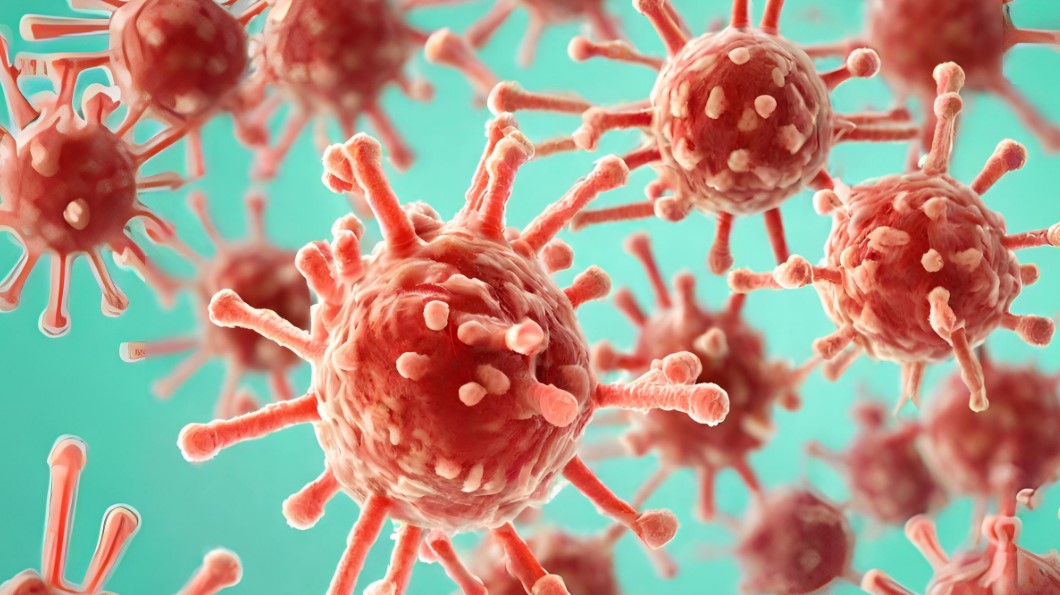 The influenza virus, commonly known as the flu, is an acute respiratory infection that poses a significant threat to global health. I will discuss its seasonal variations as well as the strains responsible for past pandemics.
The influenza virus, commonly known as the flu, is an acute respiratory infection that poses a significant threat to global health. I will discuss its seasonal variations as well as the strains responsible for past pandemics.
Seasonal Influenza Variants
I understand that seasonal influenza is a cyclic occurrence, with various strains causing illnesses each year. These variants are typically the result of minor changes in the virus’s genetic composition, known as antigenic drift.
In a typical year, influenza is responsible for numerous infections worldwide, with strains such as H1N1 and H3N2 frequently circulating among the population as per ScienceDirect. Seasonal flu can lead to severe health complications, especially in high-risk groups like the elderly, young children, and individuals with certain health conditions.
Pandemic Influenza Strains
On the other hand, pandemic influenza strains arise from a significant shift in the virus’s structure, known as antigenic shift, resulting in a novel virus to which humans have little to no immunity stated by the CDC. Notable examples include the H1N1 strain causing the 1918 influenza pandemic, which was one of the deadliest events in human history.
More recently, the 2009 H1N1 pandemic, although less severe, demonstrated that newly emerged strains could spread rapidly around the globe, necessitating robust surveillance and response mechanisms to mitigate impact.
4. Coronaviruses
Coronaviruses are a group of viruses known for causing respiratory infections in humans and animals. I’ll discuss three particularly notable strains that have impacted global health.
SARS-CoV
Severe Acute Respiratory Syndrome Coronavirus (SARS-CoV) emerged in 2002, causing a worldwide outbreak. The virus spreads through direct contact with respiratory droplets from an infected person and often leads to severe pneumonia according to a Hopkins Medicine. Containment strategies eventually succeeded in controlling the spread of SARS-CoV.
MERS-CoV
Middle East Respiratory Syndrome Coronavirus (MERS-CoV) was first reported in 2012 in Saudi Arabia. Transmission includes close contact with MERS patients or camels, and the virus causes severe respiratory illness, alongside fever, cough, and shortness of breath according to a Medical News. MERS-CoV has demonstrated a higher mortality rate than SARS-CoV, but the number of cases has remained comparatively limited.
SARS-CoV-2
The novel coronavirus SARS-CoV-2, responsible for the disease COVID-19, rapidly spread across the globe since its discovery in December 2019 as noted by the Medscape. The virus transmits through airborne particles and surfaces, leading to a wide range of symptoms from mild flu-like to severe respiratory distress. As of my knowledge cutoff, measures such as vaccination and antiviral treatments are central to controlling the COVID-19 pandemic.
By the novel coronavirus SARS-CoV-2. The virus, which led to unprecedented global health crises, has seen mutations resulting in multiple variants. These variants have differed in transmissibility and severity, prompting ongoing adjustments in public health strategies. Vaccination campaigns have been widespread and have played a crucial role in reducing the severity and mortality of the disease.
However, the virus continues to pose challenges due to its evolving nature. Efforts to monitor these changes, adapt vaccines, and implement effective treatment protocols remain key components of the global health response. Public health authorities continue to emphasize the importance of vaccination, along with other preventive measures, to manage and mitigate the impacts of COVID-19.
5. Hepatitis Viruses
Hepatitis viruses cause liver inflammation and can lead to severe health issues, including cirrhosis and liver cancer. They range from mild to life-threatening.
Hepatitis A and E
I understand that Hepatitis A (HAV) and Hepatitis E (HEV) are usually spread through ingestion of contaminated food or water. Hepatitis A is prevalent in areas with poor sanitation and can cause acute liver disease, which although usually self-limiting, can rarely be fatal. On the other hand, Hepatitis E, while less common in developed countries, poses a high risk of severe complications in pregnant women.
Hepatitis B and C
Hepatitis B (HBV) and Hepatitis C (HCV) are of particular concern as they can lead to chronic disease and have long-term sequelae. Hepatitis B is transmitted through exposure to infected blood and bodily fluids, and it’s noteworthy that a preventative vaccine exists for HBV. In sharp contrast, although no vaccine is available for HCV, which also spreads through blood-to-blood contact, advancements in medical treatments have significantly improved the curability of this virus according to NCBI.
6. Rabies Virus
 Rabies is a vaccine-preventable viral disease that primarily spreads through the saliva of infected animals, typically via bites or scratches. I understand that rabies occurs in more than 150 countries and territories, posing a threat primarily in Asia and Africa according to WHO in Africa.
Rabies is a vaccine-preventable viral disease that primarily spreads through the saliva of infected animals, typically via bites or scratches. I understand that rabies occurs in more than 150 countries and territories, posing a threat primarily in Asia and Africa according to WHO in Africa.
The virus infects the central nervous system, leading to disease in the brain and ultimately death if post-exposure prophylaxis is not administered promptly according to NFDI. The incubation period can be prolonged, ranging from weeks to years, but once clinical symptoms appear, rabies is nearly always fatal.
Symptoms begin with nonspecific signs like fever and headache and progress to more severe neurological symptoms, including:
- Hyperactivity
- Confusion
- Paralysis
- Hydrophobia (fear of water)
- Difficulty swallowing
Preventative measures for rabies include:
- Vaccination of domestic animals
- Post-exposure prophylaxis (PEP) for humans after potential exposure
- Public health education on avoiding contact with wild animals
It’s critical to seek medical attention immediately after a possible exposure to rabies, as prompt PEP can prevent the onset of symptoms and death. The World Health Organization provides more details on the rabies virus, including key facts and prevention strategies.
7. Hantaviruses
Hantaviruses are a group of viruses carried by rodents. I recognize these as significant because they can cause two distinct types of disease in humans: hemorrhagic fever with renal syndrome (HFRS) and hantavirus pulmonary syndrome (HPS) as per Taylor & Francis Online. My knowledge indicates that hantaviruses have a worldwide distribution, with various strains prevalent in different parts of the world. For instance, the Sin Nombre virus, prevalent in North America, is particularly known to cause HPS and is primarily spread by the deer mouse.
Transmission: People typically contract hantaviruses through contact with rodent urine, droppings, or saliva. Areas infested with rodents can present a higher risk, especially when these substances are aerosolized and inhaled. However, cases among travelers are uncommon, which suggests that brief exposures are less likely to lead to infection.
As for the specific symptoms and progression, they vary by the type of disease:
- HFRS: can range from mild to severe and usually manifests with flu-like symptoms before progressing to serious complications such as kidney failure.
- HPS: initially presents similarly, but I know it can rapidly progress to severe respiratory distress and, in some cases, can be fatal.
Regarding prevention, I recognize that maintaining good hygiene in areas with rodent populations and controlling rodent infestation are essential steps to reduce the risk of hantavirus transmission..
In 2024, there is an increased emphasis on integrating environmental management and public health strategies to reduce the risk of hantavirus infections. This includes efforts to improve sanitation, reduce rodent harborage in human dwellings, and educate the public on avoiding contact with rodents. Research into vaccine development and more effective treatment options for hantavirus infections is ongoing, reflecting a continued commitment to addressing this public health challenge.
8. Dengue Virus
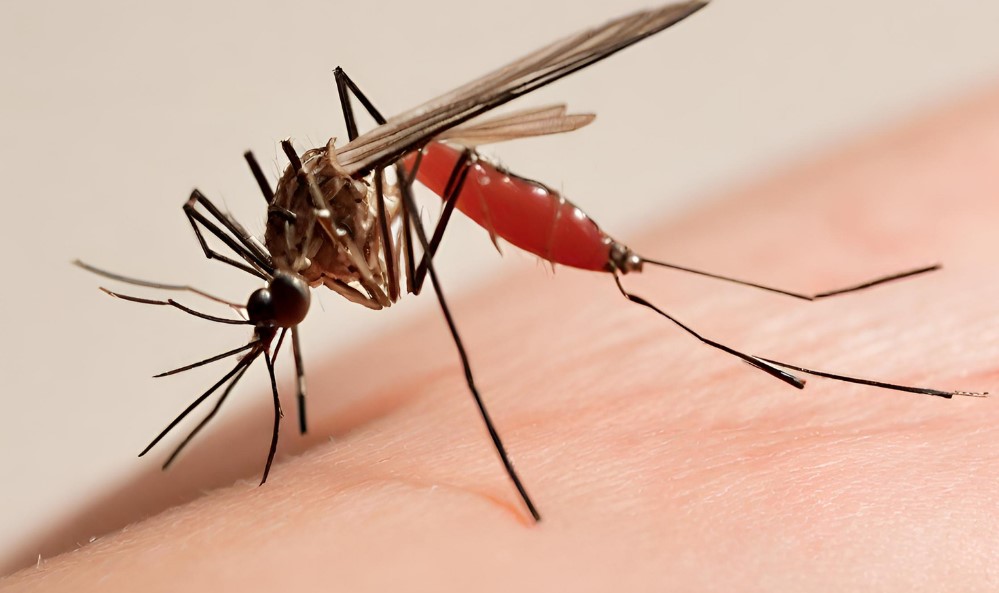 Dengue virus (DENV) is primarily spread to humans through the bites of infected Aedes mosquitoes, specifically Aedes aegypti and Aedes albopictus as per study of Parasites And Vectors. I find it important to note that the virus belongs to the family Flaviviridae and comprises four distinct but closely related serotypes (DENV-1 to DENV-4). A potential fifth has been reported, yet confirmation is pending.
Dengue virus (DENV) is primarily spread to humans through the bites of infected Aedes mosquitoes, specifically Aedes aegypti and Aedes albopictus as per study of Parasites And Vectors. I find it important to note that the virus belongs to the family Flaviviridae and comprises four distinct but closely related serotypes (DENV-1 to DENV-4). A potential fifth has been reported, yet confirmation is pending.
Below are key characteristics and impacts of the dengue virus:
- Transmission: I understand that the primary method of transmission is via Aedes mosquito bites.
- Infection: Once infected, individuals may experience symptoms ranging from mild dengue fever to severe forms such as dengue hemorrhagic fever (DHF) and dengue shock syndrome (DSS).
- Prevalence: I noted that dengue’s global prevalence is notable, with half of the world’s population at risk and an estimated 100-400 million infections yearly.
In terms of geographic distribution, while dengue is most prevalent in tropical and subtropical climates, I’ve observed that cases have expanded into more temperate regions over time. The year 2024 saw substantial infection rates, with over 4.5 million cases and notable outbreaks in various countries. My understanding is that factors contributing to the spread include urbanization, global travel, and climate change, which influences mosquito populations.
Ongoing research is critical for developing more effective vaccines and treatments to combat the disease, which currently relies on vector control and supportive care for management.
9. Marburg Virus
Marburg virus is a highly infectious pathogen that causes Marburg virus disease (MVD), a form of viral hemorrhagic fever. The virus belongs to the Filoviridae family, which also includes the better-known Ebola virus. I would like to emphasize that the Marburg virus is equally severe and often fatal as noted by PLOS. Humans contract the virus from fruit bats and can then transmit it to other humans through direct contact with bodily fluids or contaminated surfaces.
Symptoms of MVD can be particularly gruesome and, unfortunately, often fatal. Initial signs of infection are nonspecific and include:
- High fever
- Severe headache
- Malaise
As the disease progresses, patients may experience:
- Hemorrhagic manifestations
- Multi-organ dysfunction
Currently, there is no approved vaccine or antiviral treatment for Marburg virus, making prevention efforts crucial started in study of NCDC. Supportive hospital therapy, such as rehydration with oral or intravenous fluids, is the mainstay of patient management.
Historically, outbreaks have been sporadic, but each incidence garners significant concern due to the virus’s high case fatality rate, averaging around 50% according to the World Health Organization. Outbreaks require rigorous infection control measures to prevent their spread, including barrier nursing techniques and strict isolation of patients.
It is essential to have a clear understanding of the risk factors associated with Marburg virus transmission to effectively contain outbreaks when they occur. I believe that continuous monitoring and preparedness are key in mitigating the dangers posed by this virus.
10. Nipah Virus
 Nipah virus as a zoonotic virus (transmitted from animals to humans) with severe implications. It’s carried by fruit bats and can cause a range of illnesses in humans, from asymptomatic infection to acute respiratory illness and fatal encephalitis according to a study by the Lancet as per ECDC.
Nipah virus as a zoonotic virus (transmitted from animals to humans) with severe implications. It’s carried by fruit bats and can cause a range of illnesses in humans, from asymptomatic infection to acute respiratory illness and fatal encephalitis according to a study by the Lancet as per ECDC.
Transmission and Symptoms
The Nipah virus primarily transmits through direct contact with infected bats, pigs, or other infected humans. It’s notable for causing encephalitis, an inflammation of the brain, which can be fatal. Symptoms typically include:
- Fever
- Headache
- Drowsiness
- Disorientation
- Mental confusion
- Respiratory symptoms
Challenges and Treatment
There’s currently no vaccine available for either humans or animals. The primary treatment for human cases is supportive care as per study of NCDC. The high mortality rate and the lack of specific treatment make Nipah virus a public health concern, particularly in regions where outbreaks have occurred, like South Asia.
Prevention
Prevention strategies focus on avoiding exposure to sick pigs and bats in endemic areas and not consuming fruits contaminated by these bats. Public health education and surveillance are vital for controlling outbreaks.
A notable outbreak of Nipah virus occurred in Kerala, India, in 2018. This incident drew significant attention due to its high fatality rate and the challenges in containing the spread. In this outbreak, the virus was initially transmitted from fruit bats to humans and subsequently spread through close contact within families and healthcare settings. The Kerala outbreak was effectively managed through swift public health interventions, including isolation of suspected cases, robust contact tracing, and community engagement strategies.
11. Crimean-Congo Hemorrhagic Fever (CCHF) Virus
The CCHF virus is another pathogen that I find critical in terms of public health impact. It causes Crimean-Congo hemorrhagic fever, a widespread disease in Africa, the Balkans, the Middle East, and Asia, as per the World Health Organization.
Transmission and Symptoms
CCHF is primarily transmitted to people either by tick bites or through contact with infected animal blood or tissues. Human-to-human transmission can occur resulting from close contact with the blood, secretions, organs, or other bodily fluids of infected persons.
Symptoms include:
- Sudden onset of fever
- Headache
- Muscle ache
- Nausea
- Vomiting
- Diarrhea
- Rash
As the illness progresses, severe bleeding can occur, leading to significant mortality rates.
Treatment and Prevention
Treatment is mostly supportive. An antiviral drug, Ribavirin, has been used to treat CCHF virus infection with some effectiveness noted by Cochrane. Preventive measures include controlling ticks on animals and avoiding areas where ticks are abundant.
Although I have been fortunate not to have been directly affected by the CCHF virus, my family’s roots in the Balkans have brought me close to many stories and experiences related to this disease. In the communities where my relatives live, the threat of CCHF has always been a concern, particularly among those working in agriculture or living in rural areas where ticks are more prevalent.
Frequently Asked Questions
In addressing some of the most pressing inquiries regarding the world’s most formidable viruses, I aim to shed light on their impact on human history and the ever-evolving landscape of viral threats.
What are the deadliest viruses that have affected humans throughout history?
Throughout history, diseases like the Spanish influenza and smallpox have taken countless lives. More recently, HIV and the H1N1 influenza strain have also been significant causes of mortality globally.
Which viruses pose the highest level of threat in 2024?
As of 2024, viruses such as COVID-19 continue to be a major concern due to their potential for new variants. Additionally, the resurgence and spread of diseases like Marburg virus are closely monitored for their high fatality rates.
Can the severity of the Marburg virus surpass that of Ebola, and why?
The Marburg virus is closely related to Ebola and both cause hemorrhagic fevers with high fatality rates. The severity of Marburg can surpass that of Ebola due to its equally high level of lethality coupled with insufficient awareness and medical preparedness.
What are the characteristics that contribute to a virus’s high fatality rate?
A high fatality rate in viruses can be attributed to factors such as rapid mutation, efficient human-to-human transmission, and resistance to existing medical treatments. For example, the lack of a cure or vaccine can make outbreaks of viruses like Ebola particularly deadly.
How do the symptoms and mortality rates compare among the most dangerous viral diseases?
Comparing viral diseases, symptoms may range from mild to severe, with mortality rates varying widely. For instance, rabies has nearly a 100% mortality rate if untreated, while others, like influenza, have lower mortality rates but cause more deaths due to widespread infection.
What measures can be taken to protect against the spread of highly contagious and lethal viruses?
To protect against the spread, it is essential to maintain proper hygiene, vaccination, and dissemination of information regarding prevention and treatment methods. Surveillance and quick response to contain outbreaks, as seen in measures taken against diseases like COVID-19, are crucial.
Final Words
In summary, it’s evident that viruses, despite their microscopic size, have a monumental impact on public health and the course of human history. The diversity in their modes of transmission, pathogenicity, and the challenges they present in terms of prevention and treatment make them formidable adversaries in the field of medical science.
From the widespread influence of viruses like influenza and HIV to the deadly outbreaks of Ebola and Marburg virus, the fight against viral diseases remains a crucial, ongoing global endeavor. The emergence of new viruses like SARS-CoV-2, causing the COVID-19 pandemic, has further underscored the need for relentless research, surveillance, and public health preparedness.
Disclaimer
Please note that the content provided here is based on personal opinions, expertise, and experiences, as well as information gathered from various online sources. It reflects an individual perspective and should be considered as a subjective interpretation of life. This narrative aims to share personal insights and experiences to offer a unique view of the city, rather than an exhaustive or universally applicable guide.













